Cataract surgery has a high success rate – over 98% – but proper aftercare is key to achieving the best results. Follow-up appointments are designed to monitor healing, prevent complications, and adjust treatment as needed. Here’s the timeline:
- 24–48 Hours Post-Surgery: The first checkup ensures your recovery is on track. Your doctor examines the eye for signs of infection, checks pressure levels, and reviews your medication routine.
- 1 Week Post-Surgery: Vision improvement is often noticeable. This visit confirms healing progress, reviews symptoms, and adjusts activity restrictions.
- 1 Month Post-Surgery: Vision typically stabilizes. Your doctor may update your glasses prescription and assess overall recovery.
- 3 Months (If Needed): For some, a final checkup ensures long-term stability and addresses late complications like posterior capsule opacification (PCO).
Consistent follow-ups are crucial for a smooth recovery. Even if your eye feels fine, skipping appointments could risk your long-term vision. Stick to your medication schedule and report unusual symptoms like severe pain, vision loss, or increased floaters immediately.
After the recovery phase, maintain your eye health with annual checkups to monitor for age-related conditions and ensure lasting results.
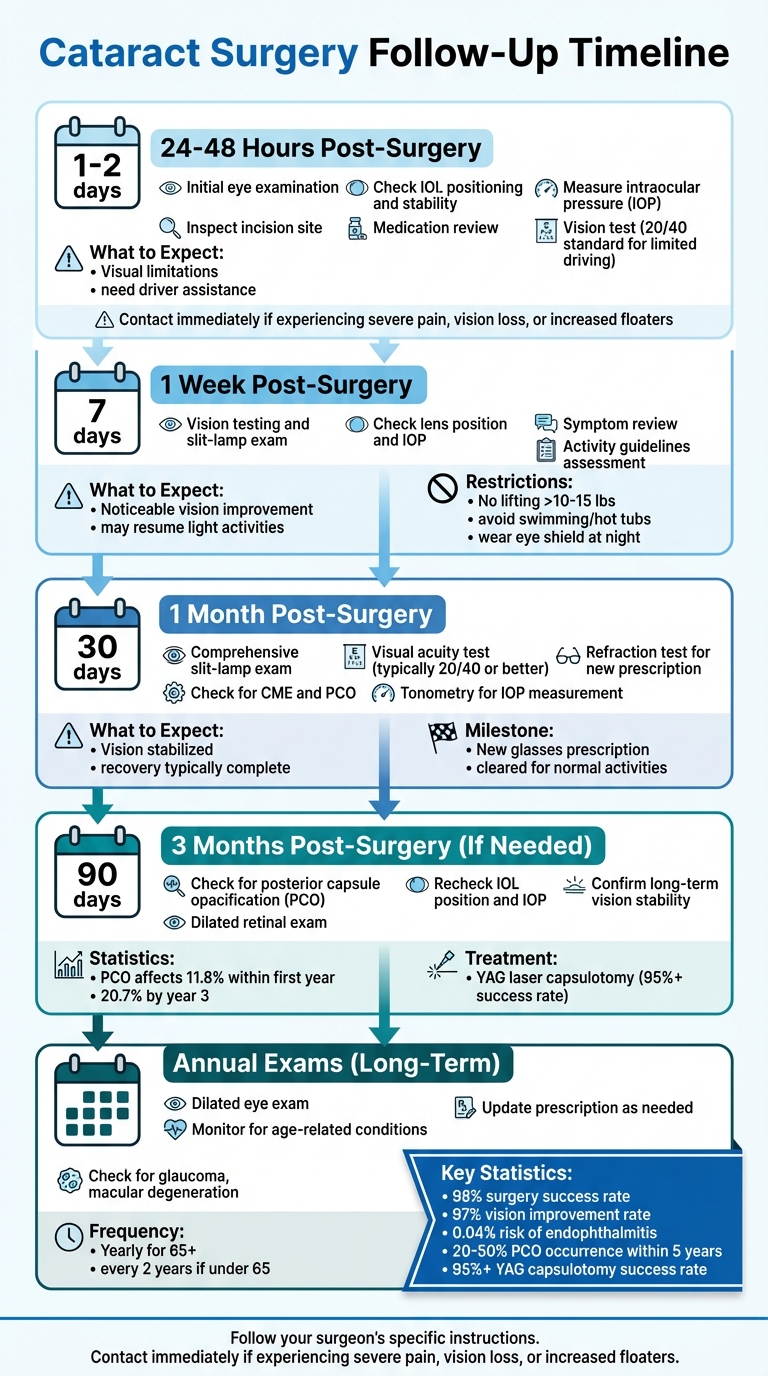
Cataract Surgery Follow-Up Timeline and Recovery Milestones
Recovery & Vision Expectations After Cataract Surgery
sbb-itb-5ef6ec9
First Follow-Up: 24-48 Hours After Surgery
Your first follow-up appointment happens 24 to 48 hours after surgery. At the Eye Center of Northern Colorado, this visit is all about ensuring your recovery is on track and catching any early complications. Since you may still have some visual limitations, make sure to arrange for someone to drive you to this appointment.
Initial Eye Examination
During this visit, your surgeon will perform a detailed examination to ensure everything is healing as expected. They’ll check that your intraocular lens (IOL) is properly centered and stable, measure your intraocular pressure (IOP) to rule out fluid buildup, and inspect the incision site for proper healing. If your IOP is elevated to 30 mm Hg or higher, your doctor may prescribe ocular anti-hypertensive medication to manage it. Thankfully, these pressure spikes typically resolve within a day or two.
Your vision will also be tested. If your visual acuity meets the 20/40 standard, you may be cleared for limited daytime driving.
"A day-one post-op visit is also useful because it offers another opportunity to go over postoperative precautions, medication regimen and allows the patient to ask questions while being in the thick of it." – Review of Optometry
The surgeon will also check for corneal clarity and monitor for any swelling. If significant swelling is found, they may adjust your steroid eye drop dosage. They’ll look for wound leaks by using a fluorescein strip to identify a Seidel sign. For those with toric lenses, the lens position will be carefully reviewed, as any rotation could interfere with your vision.
Once the physical exam is complete, the team will go over your medications to ensure you’re using them correctly.
Medication Review
Proper use of your prescribed medications is key to a smooth recovery. During this review, a technician or doctor will confirm your schedule for antibiotic and anti-inflammatory eye drops and demonstrate how to apply them correctly. Be sure to bring all your medications to this appointment so they can verify you’re taking them as directed and make any necessary adjustments. Following the medication routine is critical, as studies show the risk of endophthalmitis, a severe infection after cataract surgery, is about 0.04%.
Addressing Immediate Concerns
This visit is also your chance to talk about any discomfort or unusual symptoms. It’s normal to experience sensations like grittiness, mild redness, or light sensitivity at this stage. Using artificial tears can help with dryness, while wearing dark sunglasses outdoors can reduce light sensitivity.
That said, certain symptoms require immediate attention. Severe pain, sudden vision loss, or a noticeable increase in floaters are not typical and should be reported to your doctor right away. For mild soreness, over-the-counter pain relievers like acetaminophen or ibuprofen are usually enough. Your doctor will also remind you to continue wearing your protective eye shield at night to avoid accidental rubbing.
It’s also common for your vision to feel blurry or inconsistent during this period. This is simply your brain and eye adjusting to the new lens, and things should clear up in the days ahead.
This first follow-up is an important step in ensuring your recovery stays on track and addressing any early concerns.
1-Week Follow-Up: Checking Healing Progress
By the one-week mark, your recovery should be well underway. Many patients report noticeable improvement in their vision by this time. This follow-up appointment ensures everything is on track and helps determine if you’re ready to ease back into your normal activities. It builds on earlier evaluations to confirm consistent healing.
Vision Testing and Symptom Review
During this visit, your surgeon will check your visual acuity and perform a slit-lamp exam to ensure the lens is properly positioned and intraocular pressure is within a safe range. You’ll also have the chance to discuss any lingering symptoms. Experiencing mild grittiness, light sensitivity, halos, or glare is common at this stage. However, if you notice severe pain, sudden vision loss, rapid blurring, flashes of light, or an increase in floaters, notify your doctor immediately. Similarly, signs of infection – such as excessive redness, swelling, or discharge – should be reported right away.
"The majority of people can safely drive by the end of week 1, but I will need to see you and check your vision to let you know when you can get back behind the wheel." – Tim Greenwell, Eye surgeon & specialist
Your medication routine will also be reviewed to ensure you’re using your prescribed drops correctly. Even if your eye feels better, it’s crucial to stick to the schedule, as these drops are typically needed for about four weeks.
Activity Guidelines
At this stage, many patients can resume light daily activities and even return to work, provided it’s not physically demanding. However, there are still some restrictions to follow for a safe recovery. Avoid lifting anything heavier than 10 to 15 pounds, and when bending, use your knees rather than your waist. To reduce the risk of infection, steer clear of swimming pools, hot tubs, and saunas, and keep soap, shampoo, and tap water out of your operated eye.
Continue wearing your protective eye shield while sleeping during the first week. When outdoors, wear sunglasses that block 100% of UV rays to manage light sensitivity and shield your eye from wind and dust. Hold off on using eye makeup for at least two weeks to prevent irritation and bacterial growth.
1-Month Follow-Up: Confirming Recovery and Vision Stability
By the one-month mark, your recovery is typically complete, and your vision should have stabilized. This follow-up visit is essential for confirming healing progress and determining if any prescription adjustments are needed.
Vision Stability and Prescription Updates
At this stage, your surgeon will conduct a thorough slit-lamp exam to evaluate the health of your eye structures and check your visual acuity, which is often 20/40 or better by this time. A refraction test will also be performed to confirm your updated prescription.
"At your one-month follow-up, your doctor will test your eyesight; if your vision has stabilized, they will give you a new glasses prescription at that time." – Griffey Eye Center
It’s a good idea to wait until this appointment before purchasing new eyewear, as this ensures your prescription is accurate and stable. Additionally, your surgeon will measure intraocular pressure using tonometry to confirm it has returned to a normal, safe range.
Once these tests are complete, your surgeon will assess your overall recovery and ensure your eyes are on track for long-term health.
Final Recovery Assessment
During this visit, your surgeon will check for potential complications, such as cystoid macular edema (CME) and posterior capsule opacification (PCO). If PCO is detected, it can be treated with a quick laser procedure.
Your medication routine will also be reviewed. By the one-month mark, many patients are able to taper off or stop using eye drops altogether. Most people are cleared to fully return to normal activities at this point, including swimming, using hot tubs, engaging in strenuous exercise, and lifting heavy objects. If you had cataract surgery in one eye, this visit is also a good time to discuss scheduling surgery for the other eye if needed.
3-Month Follow-Up (If Needed): Checking Long-Term Stability
While many patients recover fully within the first month, some may need a follow-up at the three-month mark to ensure everything has stabilized. This visit is especially useful for identifying any late-emerging issues and confirming that your vision has reached its final outcome. It builds on earlier checkups by focusing on potential complications that can arise later in the healing process.
Checking for Complications
One of the key goals of the three-month follow-up is to check for posterior capsule opacification (PCO), often called a secondary cataract. This occurs when the lens capsule behind the implanted lens becomes cloudy, which can blur vision. Statistics show that PCO affects about 11.8% of patients within the first year and increases to 20.7% by the three-year mark after surgery. If you notice symptoms like a frosted appearance in your vision or increased glare around lights, it’s important to bring these up with your surgeon.
During this visit, your doctor will also recheck the intraocular lens (IOL) position, measure intraocular pressure (IOP), and perform a dilated retinal exam to catch any late-onset issues. This is particularly crucial for patients with conditions like diabetes or other pre-existing health concerns. If PCO is detected, the typical treatment is a YAG laser capsulotomy, which has a success rate of over 95%.
"YAG capsulotomy is a highly-effective procedure that results in immediate vision improvement. It has a success rate of over 95%." – Royce R. Syracuse, MD, MBA, Horizon Eye Care
Confirming Long-Term Vision Stability
Once complications are ruled out, your surgeon will confirm that your vision has stabilized for the long term. By this stage, your eye should be fully healed, and your vision should have settled into its final state. This visit includes checking your final visual acuity and determining whether a minor glasses prescription adjustment is needed. For those with premium lenses, your doctor will also evaluate how well your brain has adapted to the new optics. By now, any glare or halos should have significantly diminished.
This follow-up also serves as a baseline for your future annual eye exams, marking the start of your long-term eye health maintenance.
Long-Term Monitoring Beyond 3 Months: Maintaining Eye Health
After the initial recovery period and the three-month checkup, the focus shifts to maintaining long-term eye health. Regular monitoring becomes essential for catching age-related issues early and keeping your vision sharp. This ongoing care starts with routine eye exams.
Annual Eye Exams
Once your eyes have fully healed, aim to schedule an annual dilated eye exam. For individuals over 65, yearly exams are especially important, as conditions like glaucoma, macular degeneration, and diabetic retinopathy are more likely to develop with age. If you’re under 65, an exam every two years is generally sufficient unless your eye doctor suggests otherwise.
These visits also help ensure your eyeglass prescription stays accurate and allow early detection of any asymptomatic conditions. Pay attention to signs like increased glare or difficulty driving at night, as these could signal the need for further evaluation.
Managing Posterior Capsule Opacification (PCO)
In addition to routine exams, it’s important to stay alert for potential complications like posterior capsule opacification (PCO). If your vision becomes cloudy or blurry again, it’s not the return of your original cataract but likely due to PCO. This common long-term issue happens when residual lens cells grow on the thin membrane holding your artificial lens, forming a cloudy layer that blocks light.
Around 20% of patients experience PCO within the first year after surgery, and the likelihood increases to between 20% and 50% within five years. Symptoms include foggy vision, halos around lights, or a frosted glass effect. If these occur, contact your eye doctor promptly.
PCO is treatable with a YAG laser capsulotomy, a quick and painless outpatient procedure that clears the cloudy film. Most patients notice improved vision within hours or by the next day. To further protect your eyes, continue wearing UV-blocking sunglasses when outdoors – they’re a simple but effective way to support long-term eye health.
The team at Eye Center of Northern Colorado offers personalized care to help you maintain your vision for years to come.
Conclusion
Following through with consistent post-surgery care is just as important as the cataract procedure itself. Make sure to attend follow-up visits at 24–48 hours, 1 week, and 1 month after surgery. These check-ins help monitor your healing progress, adjust medications as needed, and ensure the lens remains properly positioned. Cataract surgery has an impressive success rate, improving vision in about 97% of patients.
Even if your eye feels fine, follow-up appointments are vital for catching rare but serious issues, such as infections, increased eye pressure, or lens displacement, that could jeopardize your long-term vision. These visits are essential for safeguarding your recovery and avoiding complications.
Stick to your prescribed eye drop schedule, even if your symptoms seem to improve. Stopping them too soon can lead to avoidable problems. If you notice sudden vision changes, ongoing pain, or new flashes and floaters, reach out to your care team immediately.
Beyond the initial recovery phase, maintaining regular eye care is essential to preserving the benefits of your surgery. Scheduling annual eye exams helps monitor for age-related changes and conditions like posterior capsule opacification, which can develop later. This long-term care ensures that the clear vision you’ve gained continues well into the future.
The Eye Center of Northern Colorado is committed to supporting you every step of the way, helping you maintain healthy eyes and clear vision for years to come.
FAQs
What if I can’t make a follow-up appointment?
If you can’t make it to a follow-up appointment after cataract surgery, reach out to your eye care provider right away to reschedule or seek advice. These follow-ups are essential for checking your recovery and spotting any possible complications. Missing them could slow down your healing process or delay identifying problems that need attention.
When can I stop my eye drops after cataract surgery?
You can generally discontinue antibiotic eye drops about 1 to 2 weeks after cataract surgery. However, anti-inflammatory drops – like steroids or NSAIDs – are usually required for a longer period, often 3 to 6 weeks, depending on your surgeon’s recommendations. Always stick to your doctor’s instructions to support proper healing.
How do I know if blurry vision later is PCO?
Blurry vision that appears months or even years after cataract surgery could be a sign of posterior capsular opacification (PCO). This condition, a frequent complication, happens when the lens capsule becomes cloudy, leading to a gradual decline in vision. An eye doctor can evaluate the situation, confirm the diagnosis, and suggest appropriate treatment options.